
Actinomyces characteristics, taxonomy, morphology, pathogenesis
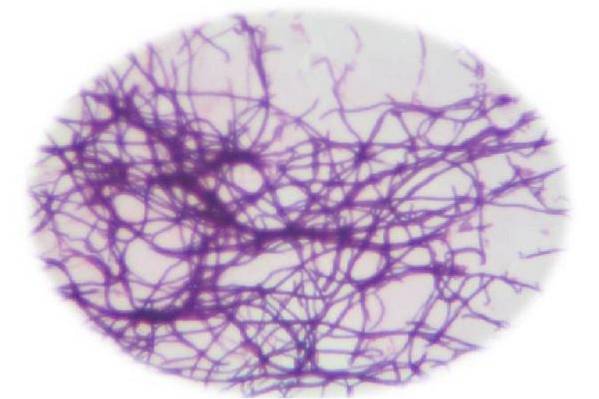
Actinomyces is a genus of bacteria composed of Gram positive rods, characterized by a filamentous growth pattern similar to the branches of a tree. In the past, this genus was confused with fungi due to its morphology, but later it was discovered that its species behaved like bacterial agents..
There are 42 identified species, but its main species are: A. israelii, A naeslundii, A. odontolyticus, A. viscosus, A. meyeri, A. pyogenes, A. georgiae, A. turicensis A. gerencseriae, A. graevenitzii.
This bacterial genus is part of the common microbiota of the gastrointestinal tract in humans and animals, ranging from the oropharynx to the colon..
Recently it was suggested that this organism could be a relatively frequent commensal, resident of the skin and mucous membranes of the urogenital region..
These species are highly adapted to living on the surface of the mucosa without causing damage. However, they can cause infections when they cross the epithelial barrier under conditions that produce oxygen tension low enough to cause their multiplication (tissue necrosis)..
Therefore, the pathologies they produce are not contagious, since the infection occurs endogenously, through trauma, surgical interventions or a foreign body..
The most frequent pathologies include orocervicofacial, thoracic and abdominopelvic actinomycosis. The disease may also appear as cutaneous actinomycosis, musculoskeletal disease, pericarditis, central nervous system (CNS) infection, or disseminated disease..
Article index
- 1 Features
- 1.1 Habitual microbiota
- 1.2 Biochemical characteristics
- 1.3 General growth characteristics
- 2 Taxonomy
- 3 Morphology
- 4 Pathologies
- 4.1 Actinomycosis
- 5 Diagnosis
- 6 Treatment
- 7 Prevention
- 8 References
Characteristics
Some species are strictly anaerobic and others are microaerophilic. They are slow growing, some strains need up to 7 days or more to make their appearance.
They grow at 35 to 37 ° C. They are not mobile, nor do they form spores. They are acid resistant bacilli, so their cell wall has some similarity to the wall of mycobacteria.
The Actinomyces have low virulence potential, causing disease only when mucosal barriers are violated, by trauma, surgery or inflammation - infection, favored by conditions of low tissue pressure of Otwo.
Infection with Actinomyces promotes pelvic invasion of other germs such as Escherichia coli, streptococci, anaerobic bacteria among others.
Habitual microbiota
They appear at an early age as oral and gastrointestinal microbiota. One study revealed that 2-month-old babies were already colonized by TO. odontolyticus in the oral cavity.
At 2 years of age there is already a great variety of species A. naeslundii, A. viscosus, A. graevenitzii, and A. gerencseriae at the time of the eruption of the primary teeth.
Actinomyces species have been reported to play a central role in the early stages of biofilm formation on teeth (dental plaque), both above (supragingival) and below (subgingival) the gum line.
This is maintained in adulthood, not being related to periodontal diseases. However, it has been found that A. turicensis is the most common Actinomyces species on the surface of the tongue in patients with halitosis, followed by A. odontolyticus, A. israelii and A. radingae.
Likewise, some species of this genus have been isolated from the female urogenital tract in the absence of actinomycetic infection. They are considered to be native microbiota, which have migrated from the perineal area or as a result of oral sex and anovaginal intercourse..
Among them are A. meyeri, A. neuii, A. radingae, A. turicensis and A. urogenitalis.
On the other hand, the following species have been isolated from urine samples: A. neuii, A. turicensis, A. urogenitalis, A. europaeus, A. odontolyticus, A. graevenitzii, A. naeslundii and A. oris since they are part of the microbiota of the female bladder.
While, A. socranski is a normal colonizer of the vagina, colon and mouth.
Biochemical characteristics
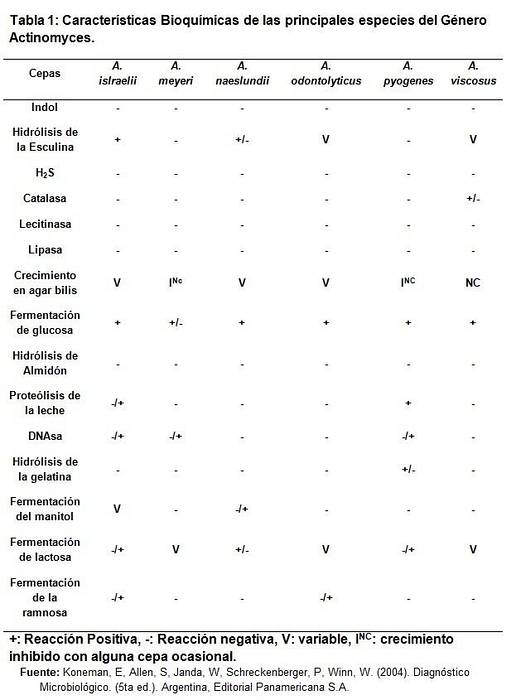

General growth characteristics
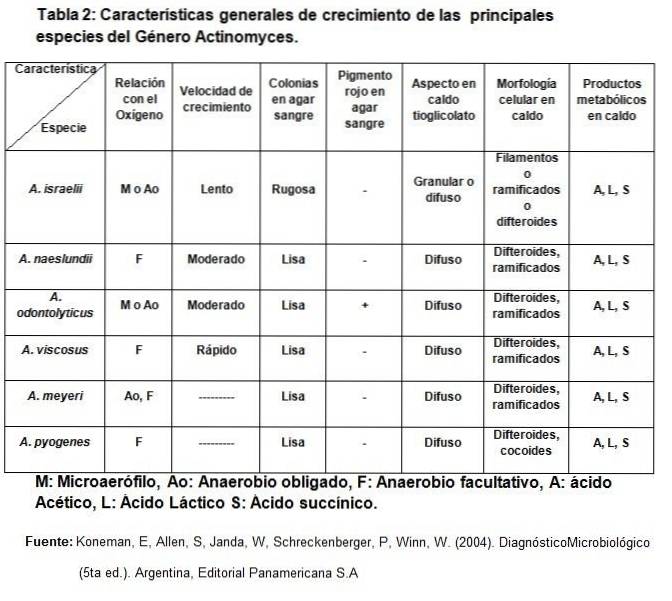
Taxonomy
Domain: Bacteria.
Phylum: Actinobacteria.
Order: Actinomycetales.
Sub-order: Actinomicineae.
Family: Actinomycetaceae.
Gender Actinomyces.
Morphology
They are Gram positive rods of 1 µm in diameter, but of variable length, since they can form branched or unbranched filaments. It can also present as short diphtheroid bacilli, or club-shaped.
Depending on the species, they can develop slowly, moderately or rapidly on blood agar. Its colonies are rough or smooth depending on the strain involved.
The color of the colonies on blood agar varies according to the species between white, greyish, red or translucent, they can be opaque or shiny and have irregular or lobed edges..
In infected human tissue they are concentrated as microcolonies, together with tissue elements, which form orange-yellow granules, called sulfurous granules because of their similarity to sulfur grains..
Pathologies
Actinomycosis
It is a chronic inflammatory and granulomatous condition that originates in the tissues adjacent to the mucosal surfaces. Lesions follow a slow course of deep and lateral expansion with considerable induration and draining fistulas.
Its exact nature depends on the organs and structures involved. It is more common in adult patients and in males..
Signs and symptoms can be very nonspecific such as swelling, cough, low fever, and weight loss.
Diagnosis is often difficult, since when observing a growing fibrotic mass, which spreads through the planes of the tissues, it can be confused with a malignant tumor.
Types of actinomycosis include:
Cervicofacial actinomycosis
It is related to poor dental hygiene, tooth extraction, or trauma to the mouth or jaw. Produces lymphadenopathy.
The infection can lead to bisphosphonate-related osteonecrosis of the jaw.
The most isolated species in this type of injury are A. israelii (42%), A. gerencseriae (26.7%), A. naeslundii Y A. viscosus (9%), while A. odontolyticus, A. meyeri, A. georgiae Y A. neuii subsp. neuii recover occasionally.
Thoracic actinomycosis
They are unusual and come from the traumatic aspiration or introduction of infected material from the oropharynx that leads to erosion through the pleura, thorax, or abdominal wall. It can also enter the bloodstream but is rarer.
In the case of thoracic actinomycosis, it is necessary to make a differential diagnosis with lung cancer, pneumonia and tuberculosis.
Actinomyces graevenitzii has a special predilection for the thoracic area, being the main Actinomyces isolated from this type of infection.
However, A. meyeri, A. israelii, A. odontolyticus Y A. cardiffensis have recovered from actinomycotic lesions at pulmonary sites and sporadically A. naeslundii and A. viscosus.
Abdominal-pelvic actinomycosis
Abdominal actinomycosis mainly presents as a consequence of invasive procedures such as laparoscopic cholecystectomy with missing gallstones or abdominal infections such as appendicitis.
While pelvic actinomycosis has been associated with the prolonged use of intrauterine contraceptive devices (chronic endometritis). This is due to the fact that the microorganism grows in a synthetic intrauterine medium, uniting and forming spider-shaped colonies until establishing a porous biofilm..
Another form of infection is after certain manipulations, such as transvaginal oocyte retrieval, which can lead to a Tubo-ovarian abscess caused by Actinomyces..
Actinomyces naeslundii, A. meyeri, A. israelii, A. funkei, A. odontolyticus Y A. turicensis are the most isolated in abdominal affectations.
In the pelvics A. israelii A. odontolyticus, A. urogenitalis, A. hongkongensis, A. cardiffensis, and A. turicensis are the most frequent.
Cutaneous actinomycosis
Cutaneous actinomycosis is usually a secondary infectious process with an underlying focus in the deeper tissues, with a tendency to the formation of fistulas through which the characteristic granules flow..
They may rarely appear as a result of hematogenous spread of an actinomycotic lesion anywhere in the body..
Manifestations with single or multiple draining sinuses can occur in various parts of the body, including the face, chest, diaphragm, hip, as well as the upper and lower extremities..
Actinomyces meyeri and A. viscosus have been the most frequently isolated strains in cutaneous actinomycosis.
Musculoskeletal actinomycosis
It is possible to see cases of osteomyelitis in the spine; the body can isolate the cerebrospinal fluid and the entire spinal cord, which can leave the patient with severe neurological symptoms.
Actinomyces israelii Y A. meyeri are the most frequent in this case.
Cerebral actinomycosis
Actinomycotic lesions in the central nervous system cause is the most serious form of actinomycosis.
Actinomyces organisms generally gain access to this area, either by hematogenous spread from remote sites or directly from local actinomycotic lesions on the head. The disease usually appears as a single or multiple brain abscesses.
The possibility of actinomycosis in the CNS should be suspected, especially in patients with neurological symptoms who have a history of actinomycosis in other parts of the body..
Actinomyces israelii Y A. naeslundii are the most important species in this type of injury.
Diagnosis
Diagnosis is based on the nature of the injury, the course of slow progress, and a history of trauma or disease predisposing to mucosal invasion by Actinomyces..
Diagnosis is difficult because microorganisms are generally rare in pus, as they are concentrated in microcolonies of sulfurous granules deeply hidden in indurated tissue..
On the other hand, these lesions are usually contaminated with other bacteria, mainly Gram negative bacilli, which deviate or confuse the real etiological diagnosis, if an aerobic culture is taken into account..
The infallible diagnosis is given by biopsy (histopathological study) if it is possible to observe the sulfur granules, they are of diagnostic value.
For the histopathological study, the granules are crushed, stained with Gram and observed under a microscope..
The study will reveal a center of typical Gram-positive intertwined branching filaments, with individual bacilli branching at the periphery, surrounded by inflammatory cells, mainly polymorphonuclear neutrophils..
However, it may be necessary to examine several samples until the granules are observed, as they are scarce..
Treatment
The first thing is to debride the lesion and then place the antibiotic treatment.
Penicillin G is the treatment of choice for actinomycosis. Also ampicillin, doxycycline, erythromycin, and clindamycin are active. Penicillin treatment should be prolonged (6 to 12 months) and with high doses.
Prevention
It is important that doctors indicate prophylactic treatment every time they perform surgical maneuvers in the oral cavity and in the gastrointestinal tract..
In this way, the invasion and progression of diseases caused by Actinomyces can be avoided..
The prognosis is generally excellent if the diagnosis is made and treatment is adhered to..
References
- Bouza Y, Jam B, Tartabull Y. Pulmonary actinomycosis. Presentation of a case. Medisur 2015; 13 (6): 795-800. Available at: scielo.sld.
- Actinomyces. Wikipedia, The Free Encyclopedia. 30 May 2018, 17:49 UTC. 24 Sep 2018, 22:07 en.wikipedia.org
- Sánchez J. Mercado N, Chilaca F, Rivera J. IUD use associated with secondary infection by Actinomyces in female genital tract. Rev Esp Patol. 2004; 37 (4): 383-390.
- López-Olmos J, Gasull J. and Vivar B. Actinomyces and mixed infections in cervicovaginal cytology, in IUD carriers. Clin Invest Gin Obst. 2010; 37 (4): 134-140
- Cardona J, Herrera D, Valencia M. Prevalence of Actinomyces spp and distribution according to some demographic and clinical factors, Medellín-Colombia 2010-2012. iMedPub Journals Arch med. 2015; 11 (4): 1-9.
- Sharma S, Valentino III DJ. Actinomycosis. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2018.
- Ryan KJ, Ray C. Sherris. MicrobiologyMedical, 6th Edition McGraw-Hill, New York, U.S.A; 2010.
- Koneman, E, Allen, S, Janda, W, Schreckenberger, P, Winn, W. (2004). Microbiological Diagnosis. (5th ed.). Argentina, Editorial Panamericana S.A.



Yet No Comments