
Actinomyces israelii characteristics, morphology, pathogenesis
Actinomyces israelii it is the most important species of bacteria of the Genus Actinomyces. It was described by Kruse in 1896 and was previously known by the name Israeli Streptothrix.
Due to their morphological characteristics, at some point the members of this genus were mistaken for fungi. However, when they observed that they responded satisfactorily to antibiotic treatment, they were classified within the Bacteria Domain.
Actinomyces israelii It is worldwide distributed and the most frequent pathology that causes is pelvic actinomycosis, associated with the use of intrauterine devices for a long time. However, other species can also originate it, such as A. gerencseriae and A. naeslundii, among other species of bacteria.
The prevalence for this group of women varies according to the time of use of the device, reporting figures of 7%, 19%, 57% and 90%, being the group with age between 35 and 40 years those that present the highest frequency of genital actinomycosis.
Article index
- 1 Features
- 2 Taxonomy
- 3 Morphology
- 4 Pathologies
- 4.1 Cervicofacial actinomycosis
- 4.2 Pelvic actinomycosis
- 4.3 Actinomycosis of the respiratory tract
- 4.4 Pulmonary actinomycosis
- 4.5 Bronchial actinomycosis
- 4.6 Laryngeal actinomycosis
- 4.7 Osteoradionecrosis
- 5 Diagnosis
- 6 Treatment
- 7 Forecast
- 8 References
Characteristics
Actinomyces israelii are bacteria that live in a saprophytic way, mainly in the oral cavity and tonsillar crypts.
They are obligate anaerobes or microaerophiles, they are not mobile, they do not form spores and they are acid resistant under the Zielh Neelsen stain.
Pathologies caused by Actinomyces israelii they are due to an endogenous focus, spreading to normally sterile areas. This rules out that it is contagious from one person to another..
In addition, it requires special conditions for the infection to occur, that is, there must be an eruption of the mucosa where it lives, so that the microorganism invades deep tissues.
It can affect all age groups, without work or seasonal predilection.
The Actinomyces produce infections of orogenital origin. Oral sex, fellatio and cunnilingus take the Actinomyces from the oral cavity to the genitals. Rectal intercourse carries microorganisms from the intestinal system to the cervix.
Taxonomy
Domain: Bacteria.
Phylum: Actinobacteria.
Order: Actinomycetales.
Sub-order: Actinomicineae.
Family: Actinomycetaceae.
Gender Actinomyces.
Species: israelii.
Morphology
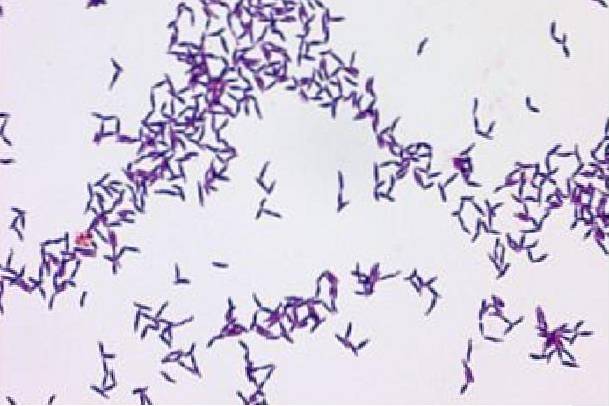
They are Gram-positive branched bacilli, which often present with a filamentary appearance on Gram stain. On blood agar the colonies are white and rough.
Under the electron microscope, the ultrastructures of Actinomyces israelii. It reveals the presence of hair-like fimbriae protruding through a thick surface coating..
For its part, the thin section reveals a Gram-positive cell wall surrounded by a diffuse outer coating. These structures are believed to be important for the pathogenicity of A. israelii.
Pathologies
Actinomycosis can develop almost anywhere, as long as the mucous membrane is disrupted. Once Actinomyces invades the tissue of a violated mucous membrane, it slowly expands and becomes an abscess.
Classic actinomycosis generally occurs after trauma, dental extractions, or other similar surgical procedures, at sites where these bacteria can reside as part of the normal flora.
There are several risk factors for the development of actinomycosis. It occurs more commonly in men. Other risk factors can include poor oral hygiene and the use of intrauterine devices..
In addition, immunosuppression and other conditions, such as diabetes, alcoholism, infections with immunosuppressive agents, and the use of steroids, predispose individuals to the development of actinomycosis..
On the other hand, the concomitant presence of other organisms can play an important role in reducing oxygen tension, making it more conducive to the growth of anaerobes..
Among the most frequent pathologies are:
Cervicofacial actinomycosis
It is called a bulging jaw, it occupies 55% of actinomycosis.
Inadequate oral hygiene has been associated with major oral diseases such as severe periodontitis, which can be the entry point for the A. israelii.
Another entry point may be tooth extraction or oral trauma.
Pelvic actinomycosis
The use of the Intrauterine Device (IUD) is considered the main predisposing factor for pelvic infection in women.
It has been shown that A. israelii in the presence of copper intrauterine devices (IUDs) they cause the formation of a biological foam within the uterine cavity that contains fibrin, phagocytic cells and proteolytic enzymes.
In the case of progesterone-secreting IUDs, they produce an atrophic endometrial tunica.
These devices allow the ascent of the bacteria from the vagina to the endocervix through its projecting threads. Subsequently, it favors the damage of the endometrial mucosa, due to a foreign body reaction.
Subsequently, the microorganism invades the tissue, where low oxygen concentrations allow its growth, forming abscesses, fistulas and characteristic fibro-dense tissue such as "sulfur granules".
The clinical manifestations are characterized by brown, dark and foul-smelling leucorrhoea, menorrhagia or abnormal bleeding, fever, dyspareunia, variable pattern of inflammation with abdominal-pelvic pain, weight loss and abdominal pain.
This pathology can lead to pelvic inflammatory disease, woody pelvis, endometritis, Tubo-ovarian abscesses, sterility, liver abscesses and death if it is not diagnosed in time..
Actinomycosis of the respiratory tract
Respiratory tract actinomycosis includes pulmonary, bronchial, and laryngeal actinomycosis. Pulmonary actinomycosis is the third most common type of actinomycosis.
Pulmonary actinomycosis
Pulmonary actinomycosis is primarily a consequence of aspiration of oropharyngeal or gastrointestinal secretions. Also due to the direct or indirect extension of a cervicofacial or hematogenous infection.
In the early stages of the disease, a focal pulmonary consolidation occurs, which may be surrounded by pulmonary nodules. There are often no associated physical symptoms at this stage.
Primary pulmonary involvement can progress slowly to the formation of a peripheral mass, with or without cavitation, that could invade the adjacent tissue.
At this stage, pulmonary actinomycosis is usually characterized by a slow-growing, contiguous fibrotic lesion that passes through anatomic barriers. The mass is often mistaken for a malignant tumor.
The most common symptoms are nonspecific, similar to those of other chronic lung infections such as tuberculosis or chest cancer: mild fever, weight loss, productive cough, hemoptysis, dyspnea, and chest pain.
Pulmonary actinomycosis could cause extrapulmonary spread, extending from the lung to the pleura, mediastinum, and chest wall, with fistulas and chronic suppuration.
Bronchial actinomycosis
Bronchial actinomycosis is rare. It can occur after mucosal barrier disruption, especially in patients with an endobronchial stent, or with a bronchial foreign body aspiration (eg, from a fish bone).
Laryngeal actinomycosis
With regard to laryngeal actinomycosis, several different forms have been described. Vocal cord actinomycosis may mimic primary carcinoma or papilloma.
In patients with a history of laryngeal carcinoma and radiotherapy, actinomycosis can simulate a relapse of laryngeal cancer, since it can present as an ulcerative lesion, most of the time without abscess or sinusitis..
Osteoradionecrosis
The therapy used in oncology, with irradiation of the head and neck area, can lead to devitalization and necrosis of the jaw.
Actinomyces israelii it has been the most frequent microorganism of this genus isolated in this type of pathology.
Diagnosis
In invasive pelvic actinomycosis, it is diagnosed by pathological study of the lesion (fistulas, abscesses, masses) or the endometrium. It can be grown on blood agar or Brucella agar, however the culture is not very useful, since the sensitivity is low and it is generally polymicrobial..
Another possibility of diagnosis is through imaging techniques, although they are often confused with neoplastic processes. In the cervical cytology or Papanicolaou the presence of Actinomyces can be detected in 44% of symptomatic women.
However, in asymptomatic women, the presence of this microorganism in the Pap smear only refers to colonization, but it cannot be guaranteed that it is a disease in process..
In Pap smears, Actinomyces they look like basophilic aggregates. These can be small and without leukocyte infiltrate, or large with amorphous material and abundant leukocyte infiltrate. Radiated filaments depart from the center.
In the case of pulmonary pathologies of doubtful origin, with nonspecific symptoms, repetitively negative microbiological tests and with radiological images suspicious of pulmonary neoplasia, the existence of pulmonary actinomycosis should be considered.
Especially in smoking patients of low socioeconomic status with poor oral status. Also in immunosuppressed patients such as HIV positive, alcoholics, diabetics, transplants, etc..
Treatment
Appropriate treatment is penicillin G and drainage of actinomycotic abscesses..
In patients allergic to penicillin, macrolides (erythromycin, clarithromycin and azithromycin), clindamycin, tetracycline or doxycycline can be used..
Conventional therapy dictates treatment with an intravenous antimicrobial agent for 6 to 8 weeks, followed by treatment with an oral antimicrobial agent for 6 to 12 months..
Premature termination of antimicrobial therapy may cause relapse of actinomycosis.
Forecast
At present, the good practice of oral hygiene, the availability of antibiotics and the improvement of surgical techniques have resulted in a decrease in mortality..
References
- Bouza Y, Jam B, Tartabull Y. Pulmonary actinomycosis. Presentation of a case. Medisur 2015; 13 (6): 795-800. Available at: scielo.sld.
- Actinomyces. Wikipedia, The Free Encyclopedia. 30 May 2018, 17:49 UTC. 24 Sep 2018, 22:07 en.wikipedia.org
- Sánchez J. Mercado N, Chilaca F, Rivera J. IUD use associated with secondary infection by Actinomyces in female genital tract. Rev Esp Patol. 2004; 37 (4): 383-390.
- López-Olmos J, Gasull J. and Vivar B. Actinomyces and mixed infections in cervicovaginal cytology, in IUD carriers. Clin Invest Gin Obst. 2010; 37 (4): 134-140
- Cardona J, Herrera D, Valencia M. Prevalence of Actinomyces spp and distribution according to some demographic and clinical factors, Medellín-Colombia 2010-2012. iMedPub Journals Arch med. 2015; 11 (4): 1-9.
- Sharma S, Valentino III DJ. Actinomycosis. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2018.
- Figdor D, Davies J. Cell surface structures of Actinomyces israelii. Aust dent J. 1997; 42 (2): 125-8.
- Honda H, Bankowski MJ, Kajioka E, Chokrungvaranon N, Kim W, Gallacher ST. Thoracic Vertebral Actinomycosis: Actinomyces israelii and Fusobacterium nucleatum . Journal of Clinical Microbiology. 2008; 46 (6): 2009-2014.
- Valor F, Sénéchal A, Dupieux C, et al. Actinomycosis: etiology, clinical features, diagnosis, treatment, and management. Infection and Drug Resistance. 2014; 7: 183-197. doi: 10.2147 / IDR.S39601.
- Ryan KJ, Ray C. Sherris. MicrobiologyMedical, 6th Edition McGraw-Hill, New York, U.S.A; 2010.
- Koneman, E, Allen, S, Janda, W, Schreckenberger, P, Winn, W. (2004). Microbiological Diagnosis. (5th ed.). Argentina, Editorial Panamericana S.A.



Yet No Comments