
Prenatal Control Characteristics and Importance
The prenatal control It is the specialized gyneco-obstetric medical care performed during pregnancy to the mother-child binomial in order to detect alterations and prevent pathologies that may endanger maternal and / or fetal life.
The health of the mother during pregnancy, childbirth and the puerperium, as well as the baby in its intrauterine stage of life, is the responsibility of the obstetrician gynecologist. For this, systematic, periodic and specific controls are established for each stage of pregnancy, in order to take care of all the details and prevent future complications..
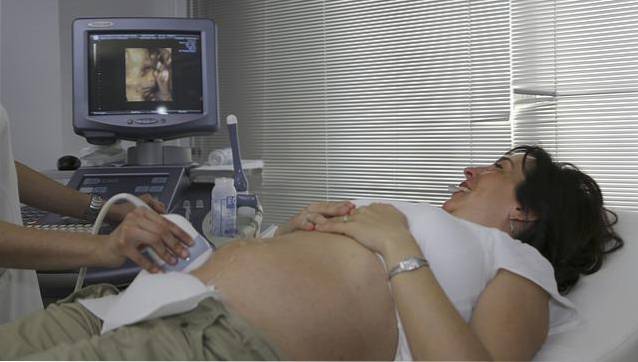
Some bibliographies have called "efficient prenatal control" to the basic principles and methods and techniques used in women during pregnancy, which are optimal in safeguarding the health of the mother and her child. The state of pregnancy brings with it a series of physiological risks that are inherent to the condition of pregnancy.
If not carefully and properly monitored, these risks can lead to unwanted situations. Although the prenatal control schedule is made to monitor the pregnancy in each of its development periods, in some women a more flexible schedule can be used if there is no risk factor that is considered to complicate the pregnancy..
However, the risks can begin in any patient without prior notice, without a similar family medical history and even in multiparous patients who had previous pregnancies without problems.
Therefore, the scheme should be applied extensively to all pregnant women, regardless of the number of pregnancies..
Article index
- 1 Importance
- 2 Features
- 2.1 Early
- 2.2 Continuity or periodicity
- 2.3 Complete or integral
- 3 References
Importance
Pregnancy, childbirth and the respective puerperium are biological conditions considered physiologically normal, since the female anatomy and physiology are prepared to face it.
However, ignorance of the factors that can positively or negatively influence pregnancy can lead to altered normal physiology of the same, since the care taken from the beginning will depend on the optimal growth and development of the future. baby.
The intention of prenatal control is to advise future parents about the risks that exist during pregnancy, and to individualize each pregnancy with genetic, modifiable and non-modifiable risk factors so that everything develops in the best possible way.
There are situations that endanger the life of the fetus that are almost imperceptible by the mother, such as decreased amniotic fluid, high blood sugar levels, high blood pressure, dehydration, anemia, blood incompatibility between mother and father, among many other uncontrollable situations.
Characteristics
Early
The woman should start prenatal care as soon as she learns of her pregnancy. Most preventable iatrogenic causes in the fetus have to do with the maternal lifestyle in the first trimester of pregnancy..
At a minimum, the first check-up should be done before week 20, and optimally the first check-up should be done before week 12.
In the first 12 weeks of gestation - or as it is also known, the first trimester of gestation - is when processes of great importance for maternal-fetal attachments occur, such as the definitive insertion of the placenta.
In this period, nutritional exchanges occur between the mother and the fetus, and there may be viral, bacterial, parasitic or toxic exchanges that may alter the development of the baby..
That is why timely control can help detect and prevent any factor that alters its normal development..
Continuity or periodicity
An efficient prenatal checkup is one whose periodicity is monthly. A pregnancy is considered as poorly controlled if it has less than 5 controls throughout the entire pregnancy.
Taking into consideration that the second half of pregnancy brings with it more flowery pathologies, it should be noted that the frequency of controls should be greater than in the first half of pregnancy.
At a minimum, the 5 controls must be carried out as follows: the first control before week 20, the second at week 24, the third at week 27, the fourth at week 33 and the fifth at week 37.
For a prenatal control to be considered optimal in terms of its periodicity, the number of controls must be 10, carried out as follows: 1 every 30 days until the eighth month, and subsequently 1 control every 15 days in months 8 and 9 , until the moment of delivery.
Complete or comprehensive
This feature is perhaps one of the most important and least flexible of all. Prenatal control should include health promotion actions, health protection actions and health recovery actions, all at the same time and focused on both the mother and the fetus..
Health promotion actions are those nonspecific actions aimed at pregnant women that seek to obtain the maximum level of health for themselves and the fetus. These actions include:
- Evaluation of fetal growth and maturation by ultrasound and obstetric examination, as well as clinical examination of the mother.
- Nutritional indication and food education to meet the physiological caloric demands of pregnancy.
- Health, hygiene, physical and psychological education to the mother and the family for the reception of the newborn.
Health protection actions are those that are specific and are aimed at the mother with the intention of reducing the risks of maternal-fetal morbidity and mortality..
For this, there are vaccination schemes (which provide active immunity to the mother and passive immunity to the baby), vitamin and mineral supplements, and control of blood glucose, hemoglobin and blood pressure values..
Finally, health recovery actions are also applied, in those in which the normal process of pregnancy has been altered.
An example of this are mothers who debut with high blood pressure figures. Preeclampsia and eclampsia is one of the pathologies secondary to high maternal tensions that produces more fetal deaths annually in developing countries.
If the control is efficient and the high blood pressure figures are diagnosed, the mother is treated so that it passes without problems until week 38. After that, a cesarean section is planned, in order to avoid further complications.
References
- Francisco A. Uganda Imaz. Practical Obstetrics. 5th Edition. Editorial Intermédica. (1981) pp. 183-195
- Group CTO. Topic 22. Gestational Evaluation. Gynecology and Obstetrics. Editorial CTO. (8th Edition. (2011) Pages 78-84
- Centers for Disease Control and Prevention. (2015). Preconception health and health care. Recovered from: cdc.gov
- March of Dimes. (2011). Your first prenatal care checkup. Recovered from: archofdimes.org
- Prenatal Control. Maternal and Child Health Project Quetzaltenango, Totonicapán and Sololá. Japan International Cooperation Agency. Recovered from: jica.go.jp


Yet No Comments