
Morganella morganii characteristics, diseases, treatments
Morganella moganii it is a Gram-negative commensal bacillus from the intestinal tract of humans, other mammals, and reptiles. Although this bacterium is widely distributed in different species, it rarely causes disease in healthy individuals, however, it is an opportunistic pathogen..
It can cause severe infections including endophthalmitis (infection affecting the eyeball), central nervous system infections, Ludwig's angina (infection of the oral floor), bacteremia, and urinary tract infection..
The Morganella moganii can develop resistance to antibiotics and although serious infections by this bacterium are rare, they have a high mortality without adequate treatment.
Its detection must be carried out by laboratory analysis, since the symptoms of the diseases it causes can be confused with those of other diseases or with those of other causative agents..
Article index
- 1 Features
- 2 Taxonomic and systematic history
- 3 Life Cycle of Morganella morganii
- 4 Diseases it can cause
- 4.1 diarrhea
- 4.2 Urinary tract infections
- 4.3 Septicemia and Bacteremia
- 4.4 Other diseases
- 5 Symptoms of contagion
- 5.1 diarrhea
- 5.2 Urinary tract infections
- 5.3 Septicemia and bacteremia
- 6 Treatments
- 6.1 diarrhea
- 6.2 Urinary tract infections
- 6.3 Septicemia and bacteremia
- 7 References
Characteristics
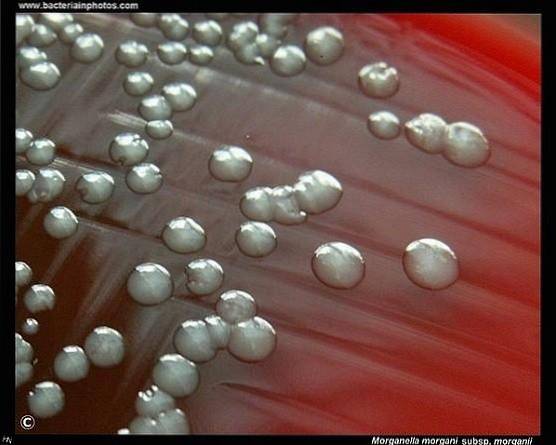
Morganella moganii It is a Gram negative, facultative anaerobic and oxidase negative bacterium, shaped like a straight bar between 0.6 and 0.7 um in diameter and 1.0 and 1.8 um in length.
Its colonies appear whitish and opaque when grown on agar plates. It is flagellated at temperatures below 30 ° C, however, at temperatures above this, it is unable to form flagella. Does not form swarms.
Taxonomic and systematic history
The gender Morganella, belonging to the Proteeae tribe, of the Enterobacteriaceae family, it was erected by Fulton in 1943 to contain, in a single, "two species" previously described, Bacillus columbensis Y Proteus morganii.
In this work Fulton demonstrated that these two species were really the same species, accepting the specific epithet of Proteus morganii, for having been the first to be described.
Indeed, Proteus morganii It had been described for the first time in 1906 by H. de R. Morgan, a British bacteriologist, who isolated the material described from the feces of infants suffering from "summer diarrhea.".
Morgan named the bacteria "Morgan's bacillus." This bacillus was later renamed as Bacillus morganii by Winslow et al. in 1919 and as Proteus morganii by Rauss in 1936.
To date the genre Morganella It is represented by two species: Morganella morganii with two subspecies (Morganella morganii morganii Y Morganella morganii sibonii) Y Morganella psychrotolerans.
Life Cycle of Morganella morganii
Morganella moganii It can be achieved in the soil and in both uncontaminated water and wastewater. This organism rapidly colonizes the intestinal tract of numerous species during their first hours of life, where it coexists as a commensal without causing damage to healthy organisms..
The bacillus, however, can thrive uncontrollably and become highly pathogenic if it accidentally penetrates (open wounds, dental extractions, surgical operations) into parts of the body where it is not normally found or if the host is immunocompromised..
Diseases it can cause
Diarrhea
Despite Morganella morganii it is frequent in the feces of healthy organisms, its incidence is notably higher in cases of diarrhea. However, it can also be caused by other pathogens such as viruses, other bacteria such as Escherichia coli, some foods and medications.
Urinary tract infections
Morganella morganii It has been involved in cases of urinary tract infections in humans, however its participation in this type of disease is lower than that of Proteus mirabilis, due to its slower growth rate in urine and the non-inducible nature of its urease.
Septicemia and Bacteremia
Among the bacteria of the tribe Proteeae, the species belonging to the genus Proteus are the most common human pathogens and cause a variety of nosocomial diseases, including urinary tract infections, septicemia, and wound infections.
Bacteremia due to Morganella morganii, for their part, they remain relatively rare. However, the latter are associated with high mortality rates, especially in those cases that do not receive adequate antibiotic therapy..
Other diseases
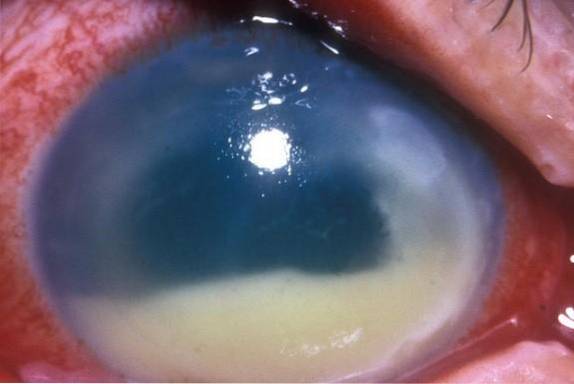
Morganella morganii It has been indicated as a causal agent of pneumonia, endophthalmitis, empyema (accumulation of pus in a body cavity), infections of surgical wounds, neonatal sepsis, spontaneous bacterial peritonitis, infections of the central nervous system and Ludwig's angina, among other diseases.
This species has also been isolated from snakes and chickens that suffer from respiratory diseases, eye injuries from spotted seals and elephant seals, septicemia in alligators, and pneumonia in jaguars and guinea pigs..
It is not clear whether in all these cases Morganella morganii was the causal agent in diseases or an opportunistic colonizer of previously diseased tissues.
Symptoms of contagion
Diarrhea
Symptoms of diarrhea caused by Morganella morgani they are similar to those caused by other agents and include a bowel movement of liquid stools three or more times a day, abdominal cramps, and nausea. They can also include blood in the stool, fever, chills, and vomiting..
Urinary tract infections
Urinary tract infections may be asymptomatic or show, among others, the following symptoms: frequent and scanty urine, cloudy, red, pink or brown in color and strong odor, constant and urgent need to urinate, burning sensation when urinating, pelvic pain in women.
Septicemia and bacteremia
Bacteremia is the presence of bacteria in the bloodstream from an infection, injury, or medical procedure. It can be asymptomatic or cause a slight fever, but can complicate into septicemia.
Septicemia is a life-threatening complication of infection. Its symptoms include: very high body temperature (greater than 38.3 ° C) or low (less than 36 ° C), more than 90 heart beats per minute, more than 20 breaths per minute.
In case of complications, chills, sensory alterations, hypotension, abdominal pain, nausea, vomiting or diarrhea may appear..
Treatments
Diarrhea
The suggested treatment is the general one for diarrhea:
- Ingest large amounts of fluids and rehydration salts to avoid dehydration.
- Avoid drinking milk.
- Do not take over-the-counter antidiarrheals.
- Rest and rest.
Urinary tract infections
For urinary tract infections caused by Morganella morganii, treatment should be carried out with oral quinolones such as ciprofloxacin. Third-generation cephalosporins and trimethoprim-sulfamethoxazole, or carbapenems, could also be used..
Septicemia and bacteremia
There is no 100% effective treatment because bacteria can develop resistance to drugs. Third or fourth generation cephalosporins with or without aminoglycosides have been suggested to treat infections caused by Morganella and reduce the possible appearance of resistance to treatment.
Carbapenems have also been used with the addition of other antimicrobials or aminoglycosides in cases of bacteremia..
For patients with allergies to these drugs, the use of quinolones such as ciprofloxacin, or high doses of trimethoprim-sulfamethoxazole and aminoglycosides is suggested..
References
- I-K. Lee, J.W. Liu (2006). Clinical characteristics and risk factors for mortality in Morganella morganii Journal of Microbiology, Immunology and Infection.
- Jamela, A.G. Ibtesam (2008). Isolation, identification, and antimicrobial susceptibility of uropathogenic Morganella morganii. Al-Kindy College Medical Journal.
- Emborg, P. Dalgaard, P. Ahrens (2006). Morganella psychrotolerans sp. nov., a histamineproducing bacterium isolated from various seafoods. International Journal of Systematic and Evolutionary Microbiology.
- Vandenberge, V. Jasson, S. Van der Heyden, P. Wattiau, S. Roels (2013). Morganella morganii associated bronchointerstitial pneumonia in a guinea pig. Vlaams Diergeneeskundig Tijdschrift.
- Manos, R. Belas (2006). The Genera Proteus, Providence, and Morganella. In: Dworkin M; Falkow, S; Rosenberg E; Schleifer, KH; Stackebrandt E (eds) The Prokaryotes. Springer, New York, NY, 245-260.
- Y. Lin, V. Kak, F. Chang. Morganella species. In Antimicrobe. Retrieved on September 1, 2018 from antimicrobe.org.



Yet No Comments