
Streptococcus sanguinis characteristics, morphology, life cycle
The Streptococcus sanguinis, formerly known as Streptococcus sanguis, It is a Gram positive facultative anaerobic bacterium that is part of dental plaque. Under normal conditions, it occurs in the mouth because it has the ability to adhere to saliva by interacting with proteins on the tooth surface..
It is an antagonist of other species of its genus that can be pathogens, such as S. mutans, which is the main promoter of caries bacteria.
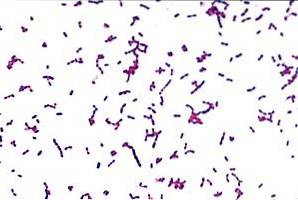
Streptococcus is a genus of Gram positive bacteria, among which we find a wide variety of species that may or may not be pathogenic for the human body..
In this diverse group of microorganisms we can find bacteria that are part of the oral or intestinal flora of humans and that have beneficial functions on the homeostasis of the organism, such as the control of pathogenic microorganisms and the production of molecules that act in physiological activities. Among them we find S. sanguinis, a bacterium of the oral cavity.
Article index
- 1 Is it pathogenic?
- 2 Biological characteristics
- 3 Morphology
- 4 Life cycle
- 5 Symptoms of contagion
- 6 Treatment for infective endocarditis caused by viridans group streptococci
- 7 Diagnostic methods for the identification of endocarditis caused by S. sanguinis
- 8 References
Is it pathogenic?
Under normal conditions, this bacterium is not pathogenic, although when there is an alteration of homeostasis in the body, there may be a decrease in the population.
This makes the oral cavity vulnerable to invasion by S. mutans and other pathogens such as Prevotella internedia, which causes gingivitis and periodontitis..
Additionally, S. sanguinis is one of the main causes of infective endocarditis of the native valve. This pathology occurs due to endovascular infection of the cardiac structures that are in contact with the blood flow.
Biological characteristics
S. sanguinis is a Gram-positive facultative anaerobic bacterium, belonging to the S. viridans group.
This bacterium is anaerobic, due to its ability to survive without oxygen, however, being facultative, it has the great capacity to use oxygen within its metabolic processes for fermentation, without being toxic to it..
S. sanguinis is a Gram positive bacterium, characterized by the presence of a cell envelope composed of a cytoplasmic membrane and a thick cell wall composed of peptidoglycans..
These two layers are joined by the junction of lipoteichoic acid molecules. Unlike Gram-negative bacteria, cell wall peptidoglycans in Gram-positive bacteria have the ability to retain the dye during Gram staining, so dark blue or violet bacteria can be seen.
The main characteristic of streptococci belonging to the S. viridans group is that they are alpha-hemolytic, which means that they produce alpha-hemolysis on blood agar, where the formation of a greenish halo around the colony can be observed..
This process is mainly due to the oxidation of hemoglobin in erythrocytes through the secretion of hydrogen peroxide (H2O2).
The ability of this bacterium to adhere to the salivary covering and the tooth surface is presented by the affinity of the components of its membrane to components of saliva such as immunoglobulin A and alpha amylase..
Morphology
The morphology of streptococci of the viridans group is very basic. Bacteria of this genus have a rounded shape, with an average size of 2 micrometers in diameter and are grouped in pairs or medium or long chains, do not have capsules and are not sporulated..
These bacteria present a gray-greenish coloration, and present the cell membrane and the cell wall composed of peptidoglycans, which are responsible for retaining the coloration in the Gram stain.
Viridans group bacteria present adhesion structures in the cell membrane, among which are fimbriae and adhesins, responsible for binding to specific receptors of the dental film.
Lifecycle
This bacterium found in dental biofilm, behaving benign under normal conditions, forms together with 700 other types of bacteria part of the normal flora of the human oral cavity..
Its colonization cycle begins between 6 and 12 months of human life and its organization in the dental biform begins with the appearance of the first tooth..
S sanguinis is associated with healthy biofilm and through the production of glucosyltransferase synthesizes lucans, hydrolyzing sucrose and transferring glucose residues.
The adhesion process to the biofilm occurs by fimbriae and adhesins. These molecules present on the bacterial surface bind to specific receptors on the components of saliva and teeth..
Being a bacterium of the oral flora, its colonization is normal and moderate, and its appearance in the biofilm is an indicator of oral health. Its decrease is associated with the appearance of pathogens such as S. mutans, which promotes the appearance of cavities.
Symptoms of contagion
In the case of the presence of this organism in the oral cavity, there are no symptoms characteristic of a pathology, because S. sanguinis is a benign bacterium that is part of the normal flora of the mouth. However, when this is the cause of infective endocarditis, various symptoms occur..
Infective endocarditis is an endovascular alteration, that is, of the endocardium, caused by several pathogens, among which we find S. aureus, S pneumoniane and streptococci of the viridans group.
In the case of S. sanguinis, the symptoms appear late at the beginning of the infection, more or less greater than 6 weeks, with a silent evolution, which does not produce pain and can be confused with another type of cardiac pathology, especially when the patient has previous heart disease.
Later, prolonged febrile peaks, fatigue, weakness, weight loss, and heart failure may be evident. Complications such as splenomegaly may occur, which is based on the increase in the size of the liver, which causes the atrophy of the organ, thrombotic hemorrhagic manifestations, cutaneous manifestations, hemorrhages in various areas of the body (hands, feet, eyes), neurological disorders , such as cerebral thrombosis, hemiplegia and psychotic pictures, among others.
Treatment for infective endocarditis caused by viridans group streptococci
The main treatment is the use of antibiotics that do not show resistance from bacteria. The use of antibiotics depends on the progression of the infection, in normal cases it takes 4 to 6 weeks.
Several studies have shown that streptococci of the viridans group, including S. sanguinis, are sensitive to penicillin. For this reason, the treatment for the infection is carried out with a combination of penicillin with other antibiotics such as gentamicin, vancomycin and ceftriaxone..
Diagnostic methods for the identification of endocarditis caused by S. sanguinis
The main diagnostic method to determine the cause of infective endocarditis caused by S. sanguinis, and in general by any other pathogen related to the pathology, is through the demonstration by culture or histopathology of cardiac abscess.
The usual laboratory studies that are performed in conjunction with histopathological analyzes are:
-Liver biometry, acute phase reactants such as C-reactive protein to indicate inflammatory conditions, kidney and liver function, general urinalysis and blood cultures.
-Additionally, chest radiographs and echocardiograms to search for myocardial abscesses or thrombi are very useful in the diagnosis..
References
- Socransky, S. S., Manganiello, A., Propas, D., Oram, V. and Houte, J. (1977). Bacteriological studies of developing supragingival dental plaque. Journal of Periodontal Research, 12: 90-106.
- Maeda, Y., Goldsmith, C. E., Coulter, W. A., Mason, C., Dooley, J. S. G., Lowery, C. J., & Moore, J. E. (2010). The viridans group streptococci. Reviews in Medical Microbiology, 21 (4).
- Truper, H. and. L. D. Clari. 1997. Taxonomic note: necessary corrections of specific epithets formed as substantives (nouns) "in apposition". Int. J. Syst. Bacteriol. 47: 908-909.
- Caufield, P. W., Dasanayake, A. P., Li, Y., Pan, Y., Hsu, J., & Hardin, J. M. (2000). Natural History of Streptococcus sanguinis in the Oral Cavity of Infants: Evidence for a Discrete Window of Infectivity. Infection and Immunity, 68 (7), 4018 LP-4023.
- Xu, P., Alves, J. M., Kitten, T., Brown, A., Chen, Z., Ozaki, L. S., ... Buck, G. A. (2007). Genome of the opportunistic pathogen Streptococcus sanguinis. Journal of Bacteriology, 189 (8), 3166-3175.
- Hernadez, F. H. (2016). Interaction of Streptococcus sanguinis on the viability and growth of Candida albicans in the oral cavity. University of Chile, Faculty of Dentistry. Assigned to Research Project: PRI-ODO 2016 04/016
- Guide for the Treatment of Infective Endocarditis. (2011). Children's Hospital of Mexico Federico Gomez. Taken from himfg.com.mx.
- Edwin & Jessen. (). BIOCHEMISTRY AND ENVIRONMENTAL MICROBIOLOGY. Alas Peruana University.
- Sánchez C. M. A, González, T. F, Ayora, T. T. R, Martínez, Z. E., Pacheco, N. A. L (2017). What are Microorganisms. Science. 68 (2).
- Ramos, P. D., & Brañez, K. (2016). Streptococcus Sanguinis and Actinomyces Viscosus Pioneer Bacteria in Dental Biofilm Formation. Kiru Magazine, 13 (2), 179-184.
- Ge, X. T., Kitten, Z., Chen, S. P., Lee, C. L., Munro., Xu, P. (2008). Identification of Streptococcus sanguinis genes required for biofilm formation and examination of their role in endocarditis virulence. (76), 2251-2259.
- Kreth J., Merritt J., Shi W., Q. F. (2005). Competition and Coexistence between Streptococcus mutans and Streptococcus sanguinis in the Dental Biofilm Competition and Coexistence between Streptococcus mutans and Streptococcus sanguinis in the Dental Biofilm. Journal of Bacteriology, 187 (21), 7193-7203.



Yet No Comments