
Nodal tuberculosis symptoms, causes, treatment

The lymph node tuberculosis It is the tuberculosis infection that, in addition to affecting the lungs, affects the lymph nodes, mainly the cervical and supraclavicular ones. It is one of the oldest diseases in the world and is caused by two species of mycobacteria, mainly Mycobacterium tuberculosis and in exceptional cases Mycobacterium bovis.
Contagion usually occurs through droplets of saliva expelled by infected patients and inhaled by healthy patients. Other forms of transmission of the tuberculosis bacillus are known, such as through the skin or the placenta, however, they are extremely rare and have no epidemiological significance..
Approximately 33% of tuberculosis cases affect not only the lungs, but also other organs. These cases are known as extrapulmonary tuberculosis..
Article index
- 1 Causes
- 2 Symptoms
- 3 Diagnostic tests
- 4 Diagnosis
- 5 Treatment
- 6 References
Causes
Tuberculous infection is usually contracted by air through droplets expelled by coughing or sneezing..
Patients with extrapulmonary tuberculosis, without pulmonary tuberculosis, do not have the capacity to be infectious by any route of transmission.
However, patients with extrapulmonary tuberculosis who also present pulmonary tuberculosis, if they can be infected by air.
Lymph node involvement by the tubercle bacillus occurs mainly in immunocompromised patients, including HIV-infected patients, children, the elderly, diabetics, alcoholics, kidney failure, transplant patients, and patients with neoplasms or on active chemotherapy.
Symptoms
Nodal tuberculosis clinically manifests the characteristic signs and symptoms of pulmonary tuberculosis (fever, sweating, weight loss, general malaise) and additionally lymphoadenitic manifestations.
However, in some cases, extrapulmonary manifestations can be expressed in isolation, requiring specific and proven diagnostic methods to demonstrate the presence of the bacillus..
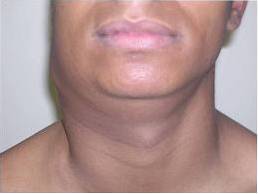
The initial manifestation is slowly evolving adenomegaly, mainly in the cervical and supraclavicular nodes, which is known as “scrofula”..
The main characteristic of this adenomegaly is that it is not painful and at the beginning each one is perfectly delimited and then begins to converge into a “mass” that continues to be painless and can sometimes fistulate and suppurate.
Diagnostic tests
The diagnostic methods of tuberculosis are mainly based on the microbiological study of respiratory secretions (sputum) to verify the presence of the bacillus..
There is also the tuberculin test or PPD, which is a purified protein derivative of tuberculosis bacilli, which is administered intradermally. If there is a local reaction, it indicates mycobacterial infection..
PPD is a skin test to detect latent tuberculosis infection in people who have not received the BCG vaccine..
To carry out this test, a PPD dose of 0.1cc VSC is administered, and after 48 - 72 hours the induration product of the injection of the subcutaneous derivative is read..
If the induration measures more than 5mm, it is considered positive in patients considered high risk such as HIV +, transplanted patients and kidney failure.
If the induration measures 10 mm, it is considered positive in patients of intermediate or moderate risk, such as those who use intravenous drugs, diabetics or children under 4 years of age.
In patients without any risk, an induration greater than 15 mm is considered positive for the presence of mycobacteria.
Diagnosis
Extrapulmonary tuberculosis is subdivided into two groups; extrapulmonary tuberculosis with bacteriological demonstration and extrapulmonary tuberculosis without bacteriological confirmation.
There are four criteria to determine the diagnosis of extrapulmonary tuberculosis without bacteriological confirmation, of which at least three must be present to establish it. The criteria are:
- Clinical and epidemiological diagnosis established by a specialist according to the location.
- Negative culture of the sample taken according to extrapulmonary location.
- Imaging findings (X-rays, MRI, Echo or CT) compatible with tuberculosis lesions.
- Pathological study.
To establish the diagnosis of lymph node tuberculosis, a Fine Needle Aspiration Puncture (FNA) of the affected lymph node is performed, which allows diagnostic confirmation in about 80% of cases..
In the same way, a previously removed lymph node can be biopsied, where bacteriological confirmation is achieved with the identification of granulomatous lesions with visible acid-fast bacilli or without their presence..
Treatment
Treatment of tuberculosis has two main goals:
-Ensure that patients are not potentially infectious and thereby interrupt transmission-
-Avoid morbidity and mortality and drug resistance in already infected patients.
The scheme for the treatment of lymph node tuberculosis depends on the category in which the patient is found and consists of two phases: an initial or bactericidal and a continuation or sterilizing.
To establish the category, factors such as age, comorbidity, access to close controlled outpatient treatment, admission to the Intensive Care Unit (ICU) or not, and whether there was a response to the first treatment scheme or not are taken into consideration..
The general scheme is the one used in patients older than 15 years of age, and consists of 4 drugs: Rifampicin, Isoniazid, Pyrazinamide and Isoniazid..
These drugs have good oral absorption and their maximum concentration is reached between 2 and 4 hours after ingestion with a total biliary / intestinal elimination in 24 hours..
The treatment regimen for both children and adults consists of an initial or bactericidal phase of two months in which the four drugs are received daily from Monday to Friday or 3 times a week: Monday, Wednesday and Friday.
In the case of hospitalized patients in the Intensive Care Unit (ICU), treatment must be received 7 days a week.
The initial phase doses are distributed as follows:
- Ethambutol 1,200 mg.
- Isoniazid 300 mg.
- Rifampicin 600 mg.
- Pyrazinamide 2 gr.
The continuation phase consists of the administration of rifampicin and isoniazid once a week for 4 months in the following doses:
- Isoniazid 600 mg.
- Rifampicin 600 mg.
In this way, the complete 6-month treatment scheme is fulfilled, which not only eliminates the pathology but also reduces the risk of recurrence to the maximum.
References
- Harrison's Principles of Internal Medicine. 18th Edition. Editorial Mc GrawHill. Volume 1. Chapter 165. Mycobacterial Diseases. P. 1340 - 1359.
- José H. Pabón. Clinical Practice Consultation - Medical. Medbook Medical Publishing House. Chapter I. Internal Medicine. Section I: Infectious Diseases. Tuberculosis. P. 25 - 37.
- Miguel Alberto Rodríguez Pérez. Cervical lymph node tuberculosis. Journal of Otorhinolaryngology and Head and Neck Surgery. Vol 72. No 1. Santiago de Chile. April 2012. Recovered from: scielo.conicyt.cl
- Shourya Hedge. Tuberculous lymphadenitis: Early diagnosis and intervention. Journal of International Oral Health. US National Library of Medicine. National Institutes of Health. Recovered from: ncbi.nlm.nih.gov
- Sharma SK, Mohan A. Extrapulmonary tuberculosis. Indian J Med Res (2004) 120: 316-53. Recovered from: ncbi.nlm.nih.gov



Yet No Comments