
Ureaplasma characteristics, morphology, pathology
Ureaplasma It is a genus of bacteria that do not have a cell wall and are characterized by hydrolyzing urea and growing in acidic media. They are microorganisms known to infect humans and other mammals, including cattle, dogs, cats, sheep, goats, raccoons, monkeys, pigs, and birds including quail, domestic chickens, and turkeys..
In humans, Ureaplasma have been isolated from the genitourinary tract of apparently healthy sexually active men and women, but it has also been found in men with urethritis and chorioamnionitis and puerperal fever in women..
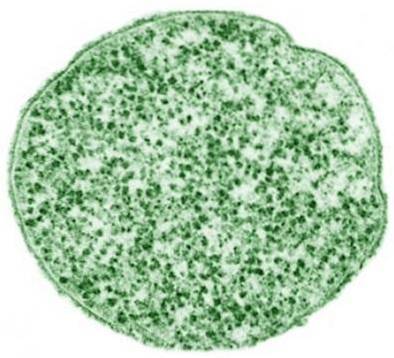
The genus Ureaplasma includes six species: U. urealyticum, U. diversum, U. gallorale, U. felinum, U. cati, U. canigenitalium. But the most important species for humans is the Ureaplasma urealyticum, since the rest of the Ureaplasmas have been found only in animals.
For example, U. diversum it is found in the respiratory and genital tracts of cattle and sheep; U. gallorale has been isolated from the conjunctiva, oropharynx, nasal cavity, and upper and lower trachea of chickens and other poultry.
While, U. felinum Y U. cati have been recovered from the respiratory tract of healthy domestic cats and U. canigenitalium found in the oral, nasal and foreskin cavity of dogs.
Article index
- 1 Features
- 2 Taxonomy
- 3 Virulence factors
- 4 Morphology
- 5 Transmission
- 6 Pathology
- 6.1 In the human
- 6.2 Pathologies in animals
- 7 Diagnosis
- 8 Treatment
- 9 References
Characteristics
The genus Ureaplasma is antigenically heterogeneous, that is, it has several serotypes and 14 in total have been described to date. These serotypes have been grouped into two subgroups or biovars.
Biovar 1 comprises serotypes 1, 3, 6 and 14 characterized by having smaller genomes. For this reason, biovar 1 is called U. parvum, which comes from the word parvo, which means little.
Likewise, biovar 2 is comprised of serotypes 2, 4, 5, 7, 8, 9, 10, 11, 12, and 13.
Ureaplasma urealyticum, as well as other microorganisms such as Mycoplasma hominis Y Chlamydia trachomatis, are considered sexually transmitted bacteria.
It is closely related to perinatal disorders and gynecological diseases and infertility.
Another important characteristic that stands out in this genre is its ability to grow in vitro at a pH between 5.5 to 6.5.
Taxonomy
Domain: Bacteria
Phylum: Firmicutes
Class: Mollicutes
Order: Mycoplasmatales
Family: Mycoplasmataceae
Genus: Ureaplasma
Virulence factors
Specifically the species U. urealyticum produces phospholipase enzymes. These enzymes hydrolyze phospholipids with the release of arachidonic acid.
Arachidonic acid released from the amniotic membrane can lead to the production of prostanglandins, triggering preterm labor during pregnancy..
Likewise, these phospholipases may also play a role in fetal lung disease when U. urealyticum reaches the respiratory tract of the fetus.
Morphology
The genus Ureaplasma resembles the genus mycoplasma in that they do not have a cell wall, but it differs from it in that they produce urease, which is why they are capable of splitting urea.
Colonies of the genus Ureaplasma are small and circular and grow into the agar..
Transmission
In the case of Ureaplasma urealyticum it is transmitted through sexual contact. Vertical transmission from the colonized mother to the term or premature neonate can also occur..
Pathology
In the human
In women
Some women may harbor U. urealyticum in vaginal fluid in relatively high concentrations due to a poor immune response. This can cause ascending infections such as subacute or chronic endometritis, leading to infertility..
In case of pregnancy, it can cause complications such as chorioamnionitis and perinatal morbidity and mortality (spontaneous abortion or premature delivery, fetal death in uterus), depending on the moment in which the infection occurs..
However, in some cases it is difficult to attribute a pathology to Ureaplasmas when they are isolated together with other pathogens recognized in the genital area such as Neisseria gonorrhoeae, Chlamydia trachomatis Y Streptococcus agalactiae.
On other occasions if their participation as pathogens is evident, for example they have been isolated U. urealyticum of blood cultures in 10% of women with postpartum or abortion fever.
Likewise, the presence of Ureaplasma in urine cultures during the first trimester of pregnancy has been associated with the development of pre-eclampsia.
In neonates
Ureaplasma urealyticum causes the death of the fetus in many cases, or influences premature birth and low birth weight. The newborn is colonized with the microorganism through contact with the mother at birth..
Some may be colonized even 3 months after birth and not develop any disease, being isolated mainly from the conjunctival and vaginal mucosa in the case of girls..
While those colonized in the respiratory tract can develop chronic lung disease, bronchopulmonary dysplasia, and systemic infection in preterm infants of colonized mothers..
It has also been recovered from CSF as a cause of meningitis in the neonatal period.
In men
On the other hand, U. urealyticum has been linked as a causative agent of non-gonococcal and non-chlamydial urethritis in men.
While its role in infertility in men is controversial.
Pathogeny
Postpartum bacteremia occurs due to the ascent of microorganisms from the site of colonization in the vagina towards the endometrium, where the microorganism causes endometritis.
Later infection of the placental membranes and amniotic fluid by Ureaplasmas occurs due to premature rupture of the fetal membranes, prolonged labor or preterm delivery.
From these sites, microorganisms enter the bloodstream during vaginal or cesarean labor.
Silent amniotic infections are even possible, i.e., U. urealyticus is capable of initiating an intense inflammatory tissue response, without associated symptoms.
Pathologies in animals
On the other hand, at the veterinary level avian Ureaplasmas appear to be non-pathogenic, however they have been associated with lesions and clinical signs that include pneumonia, aerosaculitis and peritonitis in chickens and turkeys..
Diagnosis
Currently there are semi-automated identification methods that help with diagnosis.
Mycoplasma System Plus or the A.F. Genital System are useful in identifying the microorganisms most frequently isolated by vaginal swabs, among which are Ureaplasmas..
There are also serological tests that determine specific antibodies against the microorganism..
On the other hand, there are molecular tests that can also be used for this microorganism..
Treatment
The ideal treatment is tetracycline, since it is not only effective against Ureaplasma urealyticum, but also against Chlamydia trachomatis.
However, some strains of Ureaplasma have shown resistance to this drug, in this case it is advisable to treat with a quinolone, azithromycin, minocycline or clindamycin.
Although strains of Ureaplasma urealyticum with resistance to ofloxacin and clarithromycin.
As the susceptibility patterns can change, it is important to maintain surveillance of the antimicrobial susceptibility of these microorganisms to guide the guidelines in the application of an adequate therapy..
It is important to remember that since Ureaplasma is a bacterium that lacks a cell wall, beta-lactam antibiotics and glycopeptides are not efficient in treating this microorganism..
References
- Soto E, Lemus C, Ortiz A. First isolation and identification of Ureaplasma spp and of Mycoplasma lipofaciens of commercial chickens in Mexico. Rev Mex Cienc Pecu, 2011; 2 (1): 85-92
- Ortiz C, Hechavarría C, Ley M, Álvarez G, Hernández Y. Study of Chlamydia trachomatis, Ureaplasma urealyticum Y Mycoplasma hominis in infertile patients and habitual aborters. Cuban Journal of Obstetrics and Gynecology. 2010; 36 (4) 573-584.
- Góngora A, González C, Parra L. Retrospective study in the diagnosis of Mycoplasma Y Ureaplasma in a seminal sample of 89 patients in Mexico City. Magazine of the Faculty of Medicine of the UNAM. 2015; 58 (1): 5-12
- Koneman E, Allen S, Janda W, Schreckenberger P, Winn W. (2004). Microbiological Diagnosis. (5th ed.). Argentina, Editorial Panamericana S.A.
- Ryan KJ, Ray C. (2010). Sherris. Microbiology Medical (6th edition) New York, U.S.A. McGraw-Hill Publishing House.
- Zotta C, Gómez D, Lavayén S, Galeano M. Sexually transmitted infections due to Ureaplasma urealyticum Y Mycoplasma hominis. Health (i) Science 2013; 20 (1): 37-40

Yet No Comments